Moving Upstream to Address Contributors to Toxic Stress in Pediatric Primary Care
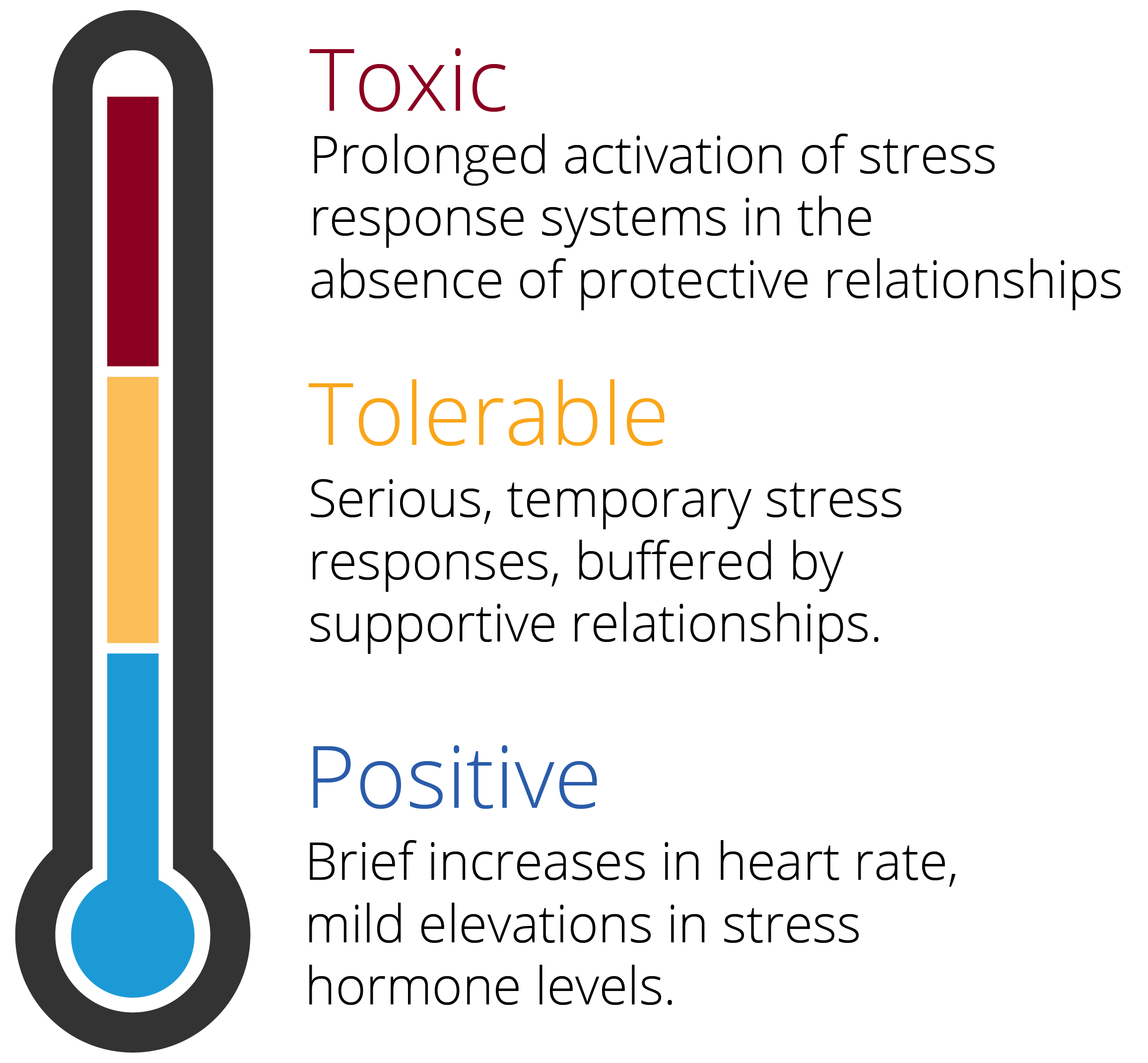
Image adapted from: https://developingchild.harvard.edu/science/key-concepts/toxic-stress
Healthcare in the U.S. is increasingly moving “upstream” to address the risk of social determinants of health. One common strategy is the early screening of needs and connection to services. Chapin Hall, in collaboration with national and local partners, is conducting an evaluation of innovations designed to promote screening for contributors to toxic stress during pediatric well-child visits and connect families to early childhood and community service providers. The first brief outlines the research questions, study design, methods, and data sources used in this study. The second brief describes the implementation experiences of clinic and partner staff. The second brief also highlights the potential of innovations like DULCE and I-SCRN to link healthcare and early childhood services and improve the quality of care families receive and strengthen relationships across service systems.
What We Did
This study examines the integration and implementation of pediatric care innovations in nine pediatric practices in 5 communities in California, Florida, and Vermont. Moving Upstream to Address Contributors to Toxic Stress in Pediatric Primary Care uses data from 51 interviews with team members who implemented the screening and referral innovations in 2018. Participants included clinicians from pediatric clinics, family specialists, behavioral health specialists, clinic administrators, legal partners, and chief medical officers.
What We Found
Results of interviews highlight multiple successes in this integrated approach to screening and referral: (1) improved relationships with families and greater willingness of families to disclose social and emotional needs; (2) development of new and stronger relationships with community and legal systems; and (3) an improvement in collaboration across staff at the clinics and a more integrated approach to family-centered care. Across sites, the focus on integrating service screening and referral into primary care resulted in positive implementation experiences for staff and improvements in the quality of care provided to families.
What It Means
Findings show the potential of community approaches to build family connectedness to the medical home and support families. Additionally, the increased willingness of families to disclose social and emotional needs demonstrates one potential benefit of screening all families for social determinants of health rather than just some. Assessing the needs of all families could support increased equity in service referral and engagement. Taken together, this brief has implications for more seamlessly integrating screening and referral innovations into clinic workflow and aligning healthcare and early childhood systems to better support healthy child development for all families.



 Thank you for your interest in Chapin Hall’s research. Please share some information to access this file.
Thank you for your interest in Chapin Hall’s research. Please share some information to access this file.