Program Integrates Adverse Childhood Experiences (ACEs) Assessment Into Primary Health Care; Connects Families with Services

Support, Connect, and Nurture (SCAN) is a program that integrates Family Development Specialist services and assessment of Adverse Childhood Experiences (ACEs) into health care provided to expectant parents and parents receiving routine health care in a Patient Centered Medical Home. The key goals of SCAN are patient education and influencing help-seeking behavior related to social determinants of health. The SCAN intervention included the following components: (a) providing families with a clinic-based Family Development Specialist, (b) connecting families with evidence-based, community parenting programs and other support resources, and (c) providing routine office visits enhanced through educated healthcare and administrative staff. SCAN is provided at Southern Colorado Family Medicine Residency in Pueblo, Colorado.
What We Did
Researchers at Chapin Hall conducted a study of the SCAN intervention over 3.5 years. The study included 899 adult patients and 23 health clinic staff who participated in the intervention from October 2015 through March 2019. The study assessed the experiences of patients and clinic staff, predominantly medical residents. At the patient-level, the extent of ACEs, resiliency and resource needs were assessed, and telephone interviews were conducted to understand more about participants’ experiences. Health visit data from electronic health records were used to examine patients’ health care utilization, specifically the use of the emergency department, and follow-through with scheduled health care visits before and after receiving SCAN (visit compliance). Clinic medical residents completed a pre-post training survey, and participated in a group interview during the last year of the study.
What We Found
- ACEs predicted depression and poorer health in adulthood.
- Resiliency buffered the relationship between ACEs and depression: ACEs are a stronger predictor of depression among adults who reported low levels of resiliency.
- SCAN was beneficial to medical providers by (1) meeting the goals of a medical home that is team-based, comprehensive, and designed around family needs and partnership; (2) reducing provider stress, which can help prevent burnout; (3) facilitating conversations about trauma and resiliency; and (4) helping providers better address family resource needs.
- Patients reported high satisfaction with both their overall healthcare visit and the portion of the visit that included the SCAN Family Development Specialist.
- Emergency department visit rates significantly decreased before and after SCAN from 1.08 to 0.84 ED visits per year on average.
What It Means
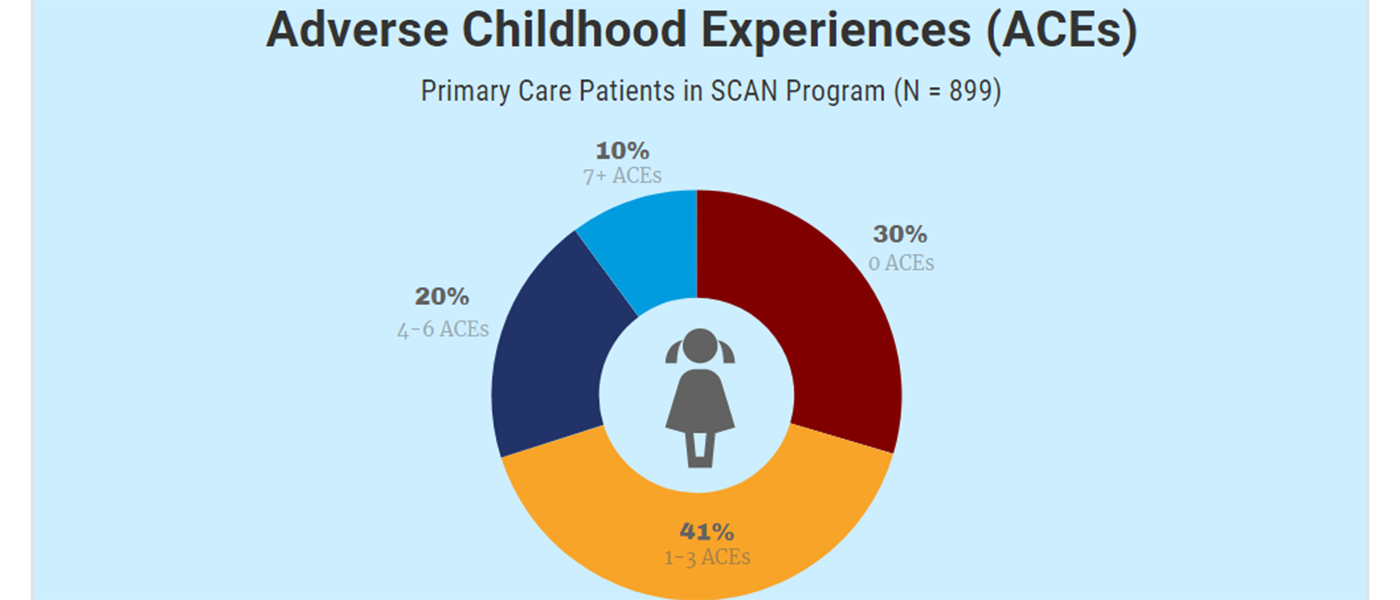
- Adverse Childhood Experiences (ACEs) are a real concern among adults seeking prenatal health care and pediatric services for their children at Southern Colorado Family Medicine Residency Clinic. SCAN patients were more than twice as likely to experience 4 or more ACEs than the CDC’s ACE Study (Felitti et al., 1998). Thus, this patient population may experience greater childhood adversity than the general population, placing them at greater risk for poor health outcomes.
- A potential intervention point is to address resiliency to mitigate the impacts of ACEs. High resiliency moderated the impact of ACEs on self-reported depression, and resiliency was related to lower rates of substance use (tobacco and alcohol), greater satisfaction with weight, healthier eating, more exercise, and greater overall health. Evidence-based programs designed to build resilience following childhood trauma should be integrated into programming between health care and community-based services.
- SCAN participants showed less emergency department use after receiving SCAN services, which reduces health care costs. This may be a result of less need for emergency care after SCAN or improved understanding of the types of concerns that require emergency care versus primary care.
- SCAN was described as alleviating physician stress, which can prevent burnout, a major issue in health care affecting the workforce, physician health, and patient care (West, Dyrbye, & Shanafelt, 2018).



 Thank you for your interest in Chapin Hall’s research. Please share some information to access this file.
Thank you for your interest in Chapin Hall’s research. Please share some information to access this file.